There are two principal categories of estimation methods for calculating infant and child mortality rates: direct and indirect. Direct methods of calculation use data on the date of birth of children, their survival status, and the dates of death or ages at death of deceased children. Indirect methods use information on survival status of children to specific cohorts of mothers, typically age cohorts or time since first birth cohorts.
The direct methods require data that are usually obtained only in specifically designed surveys with birth histories or from vital statistics systems. The indirect methods can utilize data that are commonly collected in censuses and many general surveys: the number of children ever born and the number living to women and the age or time since first birth for the women. Unlike the direct methods, the indirect methods are very dependent upon several assumptions that may or may not hold true: little or no change in fertility levels and age patterns, no change or a linear decline in mortality, and a pattern of mortality by age that conforms to known “families,” basically derived from European experience. The indirect methods are problematic in a number of settings, but especially for countries affected by HIV/AIDS mortality which have different mortality patterns.
Both types of methods can suffer from errors in data. Both methods suffer, probably equally, from the omission of deceased children. Estimation of infant mortality, using direct methods, depends on the correct reporting of age at death as under or over one year. The heaping of deaths at age 12 months is common, and to the extent that it causes a transfer of deaths across the one-year boundary, infant mortality rates may be somewhat underestimated. On the other hand, under-two and under-five mortality rates are little affected by heaping. The misreporting of birth dates can also affect direct estimates, but unless the misreporting occurs much more for deceased children, mortality rates are little affected.
Estimates of indirect methods can suffer if women do not know their ages or the age of their first child. The bias that results can be even greater if age is estimated on the basis of characteristics linked directly or indirectly to mortality levels; for example, number of children ever born. Censuses and surveys not specifically designed to gather data for mortality estimation have also been shown to be very prone to suffer from omission of reports of dead children. On the other hand, there have also been some cases where both stillbirths and live births have been included in the answer to the question on children ever born, thus leading to overestimates of mortality rates. Violations of the assumptions of the indirect methods also commonly occur.
An implicit assumption of the indirect methods is that the births of a cohort of women represent the children born in a time period. Studies have shown that births to women 20–24 (and in some cases to women 25–29) have more elements of high risk of mortality than do all children born within the last five years of a survey.
Another problem with indirect methods is the location of the estimate in time. Indirect methods estimate the probability of dying on the basis of experience that can extend over many years, resulting in an average over that period. Depending on changes in fertility and trends in mortality, the methods used to place the mortality estimate in time can be more or less in error.
Because of the number of assumptions that may or may not hold, but that need to be made to use the indirect methods and the limited amount of information that they provide, DHS has chosen to use direct estimation methods. There are three variants of direct estimation methods for estimating infant mortality rates and other rates:
A vital statistics approach in which the numbers of deaths to children under age 12 months in a particular period are divided by the numbers of births in the same period. What is estimated is a rate of mortality but not a probability; a variation in the number of births with time will change the rate without changes in the underlying probabilities. To correct this, separation factors would need to be used, which would have to come from the other variants.
A true cohort life table approach in which deaths to children under age 12 months of a specific cohort of births are divided by the number of births in that cohort. This procedure gives true probabilities of death but has the drawback that all children in the cohort must have been born at least 12 months before the survey to be fully exposed to mortality, thus not taking into account the most recent experience. This requirement of full exposure becomes more limiting the higher the age segment of interest: For under-five mortality rates, only the information on children born five or more years before the survey can be utilized. Another drawback is that true cohort rates are not specific to a particular period at death, but instead relate to the date of birth of the cohort. Therefore, the effects of events that affect several cohorts at the same time, for example, a famine appears to be spread out over time.
A synthetic cohort life table approach in which mortality probabilities for small age segments based on real cohort mortality experience are combined into the standard age segments. This approach allows full use of the most recent data and is also specific for time periods. It is the method that the DHS has chosen to use.
In the syntheticcohort life table approach, there are still severaldecisions to be made:
· The length of the individual age segments,
· How to handle the heaping of deaths at 12 months,
· How to handle deaths with incomplete information on age at death.
Length of the individual age segments
The information on age at death is recorded on the DHS questionnaire in days for less than 0-30 days, in months for 1-23 months, and in years for two years or higher. The DHS adopted the following age segments 0, 1-2, 3-5, 6-11, 12-23, 24-35, 36-47, 48-59 months (completed ages) for the calculation of the individual probabilities of dying. A different approach could have been to use monthly segments up to two years, or monthly segments up to five years with imputation of the number of months for deaths at 2 years and above. These approaches were more processing intensive when the DHS Program started in 1984, and studies done during the World Fertility Survey showed the difference to be negligible.
Heaping of deaths at 12 months
No adjustment for heaping on age at death at 12 months or one year is done for the rates presented in the survey reports. Because heaping is likely to come unequally from both sides of the one-year boundary and the correct number of deaths to reallocate is unknown, the rates are presented using the information as reported. Indeed, the extent of rounding up probably varies by country and within country, and in some cases all or most of the heaping may be due to reporting only whole year ages for children dying in the second year of life (rounding down or truncating age).
Deaths with incomplete information on age at death
For children with missing information, the ages at death have been assigned according to a “hot deck” technique in which the information of the child of the same birth order and form of reporting (days, months, or years), if available, that most nearly precedes in the data file is assigned to the child for whom age at death is missing. This is a quasi-random technique that preserves the variation of responses in the data set.
1) The neonatal mortality rate is the probability of a child exposed in a specific period dying before reaching the age of 1 month.
2) The post-neonatal mortality rate is the probability of a child exposed in a specific period on or after the age of 1 month but before reaching the age of 1 year, calculated as the difference between the infant mortality rate and the neonatal mortality rate.
3) The infant mortality rate is the probability of a child exposed in a specific period dying before reaching their first birthday.
4) The child mortality rate is the probability of a child exposed in a specific period dying on or after their first birthday but before reaching the age of five years.
5) The under-5 mortality rate is the probability (expressed as a rate per 1,000 live births) of a child exposed in a specific period dying before reaching the age of five years.
Coverage:
Population base: Live births to respondents (BR file)
Time period: Five-year or ten-year periods of time preceding the survey (v008-1 to v008-60 or v008-120 months), excluding the month of interview
Live birth: The complete expulsion or extraction from its mother of a product of conception, irrespective of the duration of the pregnancy, which, after such separation, breathes or shows any other evidence of life, such as beating of heart, pulsation of the umbilical cord, or definite movement of voluntary muscles, whether or not the umbilical cord has been cut or the placenta is attached. (WHO, 1950 and 1992).
Numerators:
Number of deaths to live-born children during specified age range and specified time period
1) Neonatal mortality: Deaths at ages 0 to 30 days, including deaths reported at age zero months
2) Post-neonatal mortality: Deaths at ages 1 to 11 months, including deaths reported at ages 31 to 99 days, defined as the difference between the infant mortality rate and the neonatal mortality rate
3) Infant mortality: Deaths at ages 0 to 11 months, including deaths reported at ages 0 to 99 days
4) Child mortality: Deaths at ages 1 to 4 years, including deaths reported at ages 12 to 59 months
5) Under-5 mortality: Deaths at ages 0 to 4 years, including deaths reported at ages 0 to 59 months and 0 to 99 days
Denominator: Number of surviving children at beginning of specified age range during the specified time period
Variables: BR file.
|
b3 |
Date of birth of child (CMC) |
|
b5 |
Child is alive (1 = Yes, 0 = No) |
|
b7 |
Age at death in months (imputed) |
|
v008 |
Date of interview (CMC) |
|
v005 |
Woman’s individual sample weight |
|
|
|
Component probabilities
Component death probabilities are first tabulated. Then the component death probabilities are combined into the mortality rates. The component death probabilities are calculated for age segments 0, 1-2, 3-5, 6-11, 12-23, 24-35, 36-47, and 48-59 months of completed age.
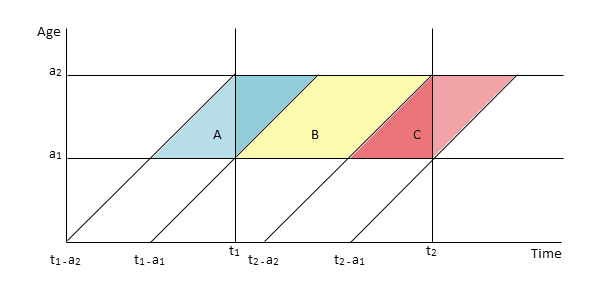
Each component death probability is defined by a time period and an age interval. Within these two parameters, three birth cohorts of children are included, as indicated in the figure below:

One cohort of children (cohort B) is completely included and two (cohorts A and C) are partially included in the time period. If the lower and upper limits of the age interval are given by a1 and a2, respectively, and the lower and upper limits of the time period are given by t1 and t2, respectively, then the three cohorts are defined as children born between dates:
· t1 - a2 and t1 - a1 (cohort A),
· t1 - a1 andt2 - a2 (cohort B), and
· t2 - a2 and t2 - a1 (cohort C)
Cohorts A and C are only partially exposed to mortality between ages a1 and a2 during time period t1 to t2. Therefore, account needs to be taken of the partial exposure. Because of the small age intervals of the component probabilities, the assumption is made that the exposure to mortality and deaths of birth cohorts A and C are well represented by taking one-half of the total exposure and one-half of the deaths (with the exception noted below).
Time periods:
The time period used is typically five years or ten years preceding the month of interview (v008-1 to v008-60, or v008-1 to v008-120), excluding the month of interview as this would only contribute a partial month. Time periods are expressed in the form [t1, t2), i.e. from t1 up to but not including t2 as follows:
0-4 years preceding the survey t1 = v008-60 t2 = v008
5-9 years preceding the survey t1 = v008-120 t2 = v008-60
10-14 years preceding the survey t1 = v008-120 t2 = v008-180
etc.
Age groups:
Age groups are expressed in the form [a1, a2), i.e. from a1 up to but not including a2 as follows:
0 a1 = 0 a2 = 1
1-2 a1 = 1 a2 = 3
3-5 a1 = 3 a2 = 6
6-11 a1 = 6 a2 = 12
12-23 a1 = 12 a2 = 24
24-35 a1 = 24 a2 = 36
36-47 a1 = 36 a2 = 48
48-59 a1 = 48 a2 = 60
For each age group and time period the numerators and denominators are calculated.
Numerators:
A. One-half of the deaths between ages a1 and a2 to children of cohort A
(a1 <= b7 < a2 & t1 - a2 <= b3 < t1 - a1), plus
B. All of deaths between ages a1 and a2 to children of cohort B
(a1 <= b7 < a2 & t1 - a1 <= b3 < t2 - a2), plus
One-half* (a1 <= b7 < a2 & t2 - a2 <= b3 < t2 - a1)
Denominators:
A. One-half of the survivors at age a1 of childrenof cohort A
((b5 = 1 or a1 <= b7) & t1 - a2 <= b3 < t1 - a1), plus
B. All of the survivors at age a1 of childrenof cohort B
((b5 = 1 or a1 <= b7) & t1 - a1 <= b3 < t2 - a2), plus
C. One-half of the deaths between ages a1 and a2 to children of cohort C
((b5 = 1 or a1 <= b7) & t2 - a2 <= b3 < t2 - a1)
Component death probabilities are calculated by dividing the numerator for each age range and time period by the denominator for that age rangeand period.
*Special exception: For the time period that ends with the date of the survey, numerators are calculated as the sum of one-half of the deaths between ages a1 and a2 to children of cohort A, plus all of deaths between ages a1 and a2 to children of cohort B, plus all of the deaths between ages a1 and a2 to children of cohort C. This change is because all of the deaths reported in the survey for cohort C for this time period represent one-half of the deaths that would have occurred to the cohort between ages a1 and a2.
Mortality rates
Neonatal mortality rate (NNMR):
This is the component death probability for 0 months of age multiplied by 1000.
Infant mortality rate (IMR):
1) Calculate the component survival probabilities by subtracting each component death probability from one.
2) Calculate the product of the component survival probabilities for 0, 1-2, 3-5, and 6-11 months of age.
3) Subtract the product from 1 and multiply by 1000 to get the infant mortality rate.
Post neonatal mortality rate (PNMR):
Subtract the neonatalmortality rate from the infant mortality rate.
Child mortality rate (CMR):
1) Calculate the component survival probabilities by subtracting each component death probability from 1.
2) Calculate the product of the component survival probabilities for 12-23, 24-35, 36-47, and 48-59 months of age.
3) Subtract the product from 1 and multiply by 1000 to get the child mortality rate.
Under-5 mortality rate (U5MR):
1) Calculate the component survival probabilities by subtracting each component death probability from 1.
2) Calculate the product of the component survival probabilities for 0, 1-2, 3-5, 6-11, 12-23, 24-35, 36-47, and 48-59 months of age.
3) Subtract the product from 1 and multiply by 1000 to get the under-five mortality rate.
Five variables are used in the calculation of infant and child mortality: date of interview, date of birth of the child, survival of the child, age at death of the child, and the women’s sampling weight. The date of interview is not allowed to be missing on the questionnaire. Survival status for children is also not allowed to be missing. If missing or unknown, the date of birth and age at death are imputed before the creation of the standard recode. See Croft, 1991 for the imputation procedures.
Typically, mortality rates are calculated for five-year periods preceding the date of the survey for national estimates. To provide stability in estimates for smaller subgroups, the ten-year period before the survey is used. To calculate the component death probabilities for the ten-year period, the numerators for the 2 five-year periods are summed, as are the denominators, before dividing the numerators by the denominators.
The reliability of mortality estimates depends upon full recall of children who have died, the absence of differential displacement of birth dates of surviving and dead children, and accurate reporting of ages at death. Previous survey results have often been characterized by some heaping of age at death at exactly 12 months or 1 year of age. Because age at death is recorded in completed months or years, deaths at 12 months are classified as child rather than infant deaths. In reality, some of these deaths may have occurred before the first birthday so that their classification as child deaths tends to negatively bias infant mortality estimates and positively bias child mortality estimates. The analyst should be aware that this may occur in DHS surveys, although the probable effect is usually modest and unlikely to bias the estimates by as much as 5 percent.
In prior rounds of the DHS Program, five-year periods were used only for national estimates, and ten-year periods were used for all disaggregations of the mortality rates. In DHS-7 and later surveys, as sample sizes have increased over the years, five-year periods are also used for mortality rates disaggregated by sex and by urban/rural residence.
Croft, T. 1991.“Date Editing and Imputation.” Demographic and Health SurveysWorld Conference Proceedings, II: 1337–1356, Columbia, Maryland: IRD/ORC Macro. https://dhsprogram.com/publications/publication-dhsg3-dhs-questionnaires-and-manuals.cfm
Moultrie T.A., R.E. Dorrington, A.G. Hill, K. Hill, I.M. Timæus and B. Zaba (eds). 2013. Tools for Demographic Estimation. Paris: International Union for the Scientific Study of Population.
http://demographicestimation.iussp.org/content/direct-estimation-child-mortality-birth-histories
Pullum, T., S. Assaf, and S. Staveteig. 2017. Comparisons of DHS Estimates of Fertility and Mortality with Other Estimates. DHS Methodological Reports No. 21. Rockville, Maryland, USA: ICF. https://www.dhsprogram.com/publications/publication-MR21-Methodological-Reports.cfm
UNICEF, WHO, World Bank, UN-DESA Population Division. Child Mortality Estimation Methods.
http://collections.plos.org/cme
UNICEF, WHO, World Bank, UN-DESA Population Division. 2017. Levels and Trends in Child Mortality. https://www.un.org/en/development/desa/population/publications/mortality/child-mortality-report-2017.asp
World Health Organization. 2018. Global reference list of 100 core health indicators. Geneva: World Health Organization. https://apps.who.int/iris/handle/10665/259951
DHS-8 Tabulation plan: Tables 8.1, 8.2, and 8.3
API Indicator IDs:
CM_ECMR_C_NNR, CM_ECMR_C_PNR, CM_ECMR_C_IMR, CM_ECMR_C_CMR, CM_ECMR_C_U5M
SDG Indicator 3.2.1: Under-five mortality rate
SDG Indicator 3.2.2: Neonatal mortality rate
WHO 100 Core Health Indicators: Under-five mortality rate
WHO 100 Core Health Indicators: Infant mortality rate
WHO 100 Core Health Indicators: Neonatal mortality rate
MICS6 Indicator CS.1: Neonatal mortality rate
MICS6 Indicator CS.2: Post-neonatal mortality rate
MICS6 Indicator CS.3: Infant mortality rate
MICS6 Indicator CS.4: Child mortality rate
MICS6 Indicator CS.5: Under-five mortality rate
UN IGME Child Mortality Estimates
R package DHS.rates: Calculate Key DHS Indicators
https://CRAN.R-project.org/package=DHS.rates